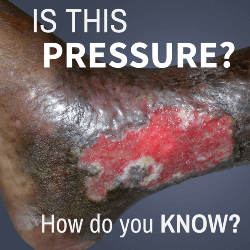
Imagine, if you will, the following scene: a wound care clinician is asked to weigh in on a lower extremity ulcer consultation, and upon arrival is told that it’s a pressure ulcer. So she seeks more information about blood flow:
Clinician #1: Tell me about the blood flow to the lower extremity.
Clinician #2: It seems okay because pulses are palpable on the foot.
Clinician #1: Are there recent Ankle Brachial Index (ABI) assessments in order to obtain a much more reliable assessment of blood flow?
Clinician #2: Um … no.
Here’s the truth
Unfortunately, this kind of conversation happens all the time, so let’s set the record straight: palpation of pulses is not a reliable assessment of blood flow to the foot. They can be misleading and leave you hanging – without the information you need to properly and safely manage the wound. An ABI will reveal what you need to know about the blood flow to the lower extremity, and give you vital clues to the underlying disease process causing the ulcer. Only when this information has been gathered can you properly develop a plan of care that will help, and not hurt, the patient.
The 2014 International Pressure Ulcer Guidelines mentions performing a vascular assessment on every lower extremity ulcer. That means, at a minimum, we need to check pulses and toe measurements, and perform an ABI. This will assist in identifying the true cause of the wound, whether it be pressure, venous, arterial, or mixed venous/arterial.
What’s this about an ABI?
An ABI is considered the gold standard of tests that can be easily performed at bedside – all you need is a blood pressure cuff and a hand-held Doppler. It is also the most useful test to assess lower extremity arterial perfusion, and compares the systolic blood pressure of the ankle to that of the arm (brachial). When should you perform ABI?
- When pulses aren’t clearly palpable or are weak
- On all patients with lower extremity ulcers
- When the ulcer is not healing
- Always before starting compression therapy
Compression therapy is the standard of care for the treatment of venous stasis ulcers. ABI results will help identify significant arterial disease and determine the amount of compression (if any) that can be applied safely. You never want to compress a lower extremity that has significant arterial flow compromise, for fear of cutting off all blood flow and causing harm to your patient.
Blood flow assessment is a must
Earlier, we used the example of a patient who has a possible “pressure ulcer.” When we are not sure of the type of wound we are treating, we need to ask some serious questions:
- Could there be arterial blood flow compromise that will make healing problematic or even unrealistic?
- Is there venous disease complicating the clinical picture that could benefit from appropriate levels of compression?
- Or is this strictly a pressure ulcer where the treatment plan will require off-loading interventions first and foremost?
The bottom line
When assessing a lower extremity ulcer, it is vital to determine the assessment of blood flow. Without the information obtained from an ABI, your care plan can be inappropriate, your goal setting can be unrealistic, and your patient could be harmed.
What do you think?
We want to know about your experiences with this topic. When do you typically obtain an ABI in practice? In long-term care settings, how often do you obtain ABI measurements? If you’re not obtaining ABIs, what are you using? Please share your experiences below.
What do you think?