Wounds in skin folds can be a challenge to prevent and, once present, involve ongoing surveillance and care.
Donald Wollheim, MD, FAPWCA, WCC, DWC, a board-certified surgeon of the American Board of Surgery, shared his insight on best practices for preventing and treating wounds in skin folds if they develop.
What Causes Wounds in Skin Folds?
Skin fold rashes and wounds, also known as intertrigo and intertriginous dermatitis, are generally due to the presence of three factors, said Wollheim:
- Friction between two layers of skin (skin against skin)
- Moisture (a buildup between these same two layers of skin)
- Lack of air flow (to evaporate the moisture)
Wollheim said when one flap of skin lays on top of another, the friction, moisture and lack of aeration causes a rash to develop between the layers of skin.
Next, the outer layer of the epidermis, called the stratum corneum, becomes inflamed because of the moisture.
Common Places Where Intertrigo Occurs
There are some common areas on the body where intertrigo can develop, Wollheim said. They include:
- Axilla: The skin of the adducted arm lies against the skin of the axilla.
- Inframammary: Underneath the breasts, when the skin of the breast lies on top of the skin of the upper abdomen and thoracic wall.
- Abdominal pannis: When the skin of the abdomen flops down on the groin and suprapubic region.
- Perineal: When the two buttocks are lying against each other or when the inferior buttocks lie against the skin of the posterior thigh.
- Genital: Between the perineum and the scrotum or between the labia.
- Interdigital: Between fingers and toes.
- Creases in the neck: Occurs when the neck is thick.
- Prosthetic limb wearers: The area where the stump of the limb rests in the socket of the prosthesis.
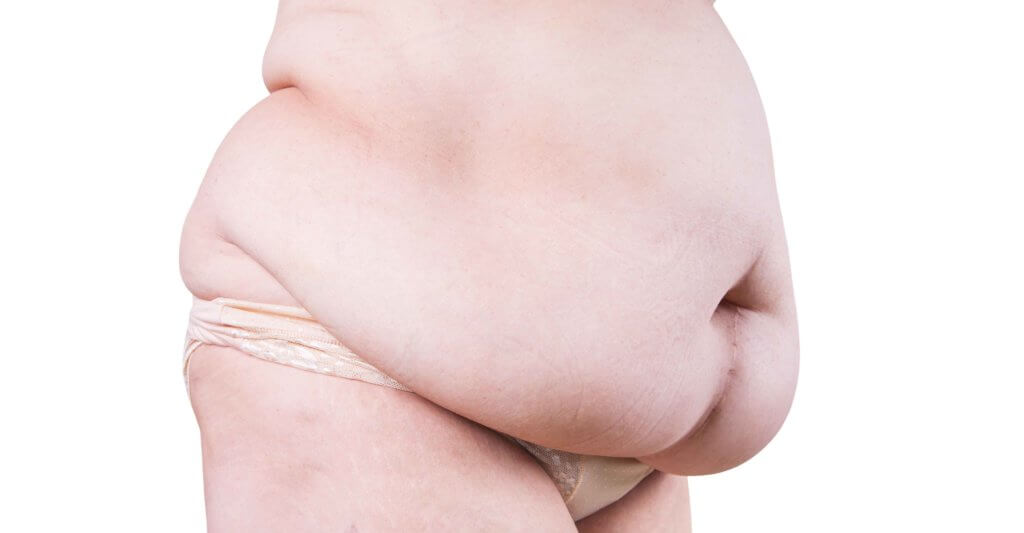
What Do Skin Fold Wounds Look Like?
Wollheim said intertrigo appears in a linear manner along the crease where the flaps meet, and looks like a half moon — with nearly an identical mirror image on each flap of the involved skin folds.
Wounds in skin folds (intertrigo) are partial thickness, meaning they involve the top two layers of skin — the epidermis and dermis. And, if a simple case, will typically appear mildly erythematous, Wollheim said.
Patient Symptoms with Intertrigo
According to Wollheim, patients with intrerigo often have some of the following symptoms:
- Burning
- Itching
- Oozing
- Maceration
- Odor
- Pain
- Satellite lesions (if a fungal infection is present)
- Red streaking leading away from the wound (if a bacterial infection is present and indicates the development of lymphangitis)
If a bacterial infection develops, it’s usually a gram-positive organism and more commonly staphylococcus or streptococcus, he said.
“When this occurs, we can also see systemic changes, in addition to lymphangitis (symptoms), such as fever, chills, nausea and vomiting,” Wollheim said.
Risk Factors for Developing Intertrigo
Wollheim said several factors can place patients at risk for developing intertrigo, such as having a history of:
- Obesity (BMI > 30)
- Diabetes
- Wearing a splint, brace or having an artificial limb or limbs
- Immune system suppression
- Living in a warm, humid climate
- Dependency on others (the very young and the elderly) to change diapers (babies/toddlers) and adult briefs (elderly)
Strategies for Preventing Wounds in Skin Folds
To prevent wounds in skin folds from occurring, Wollheim suggests the following strategies:
- Change diapers and adult briefs frequently (as soon as wet/soiled).
- Undergarments should be loose (not tight).
- Use antiperspirants in the axilla.
- Look for body soaps with a pH of 7.0 (don’t use alkaline soaps with higher pH).
- Wash and apply topicals with a light touch (avoid vigorous rubbing of skin).
- Consider using a hand-held hair dryer on the “cool” setting to use in vulnerable areas, such as the abdominal pannis.
- Take a “brief” holiday — take breaks from wearing diapers (kids) and briefs (adults) whenever possible to allow for aeration. Use bed pads during these times.
- Work to maintain blood glucose levels within normal range for patients with diabetes. Bacteria and fungi use blood glucose as an energy source.
Once intertrigo develops, Wollheim said it is important to identify the cause to correct the problem.
“If the cause is too much friction, you want to reduce the friction,” he said. “If the root cause is too much moisture, work to reduce the moisture in the affected area.”
Recommended products for intertrigo treatment
Some examples of treatment products Wollheim suggests, depending on the patient and his or her medical history, include:
- Zinc oxide, which also is an antimicrobial and can provide a good barrier.
- A polyester-based, moisture-wicking antimicrobial fabric placed between skin folds (an example is InterDry)
- Antimicrobial Kerlix dressings (AMD Kerlix), which should be changed frequently.
- Aluminum acetate solution to calm the skin and reduce redness and swelling.
- Low-dose steroids to control itching.
If a secondary bacterial infection develops, such as a cellulitis or lymphangitis, Wollheim said it is essential to recognize, diagnose and treat it as soon as possible.
Learn more in our course on Skin and Wound Management today.
Want to learn more about Skin and Wound Care?
Get Started →What do you think?

