As a wound care clinician, you may be called to work in a burn unit or be consulted on burn wounds. If that is not your normal work setting, it can be overwhelming.
Our purpose in this article is to address the fundamentals and provide a solid working knowledge of how to manage burn wounds.
Let’s start with terminology. The American Burn Association changed the classification of burns from the traditional first-, second-, third-, and fourth-degree burns to the following:
Classification of Burns
Superficial (first degree)
Damage is limited to the epidermis only. No loss of tissue. Manifests as erythema, hyperemia, and pain with no blistering. Examples are sunburn and hot liquid burns.
Superficial partial thickness (second degree)
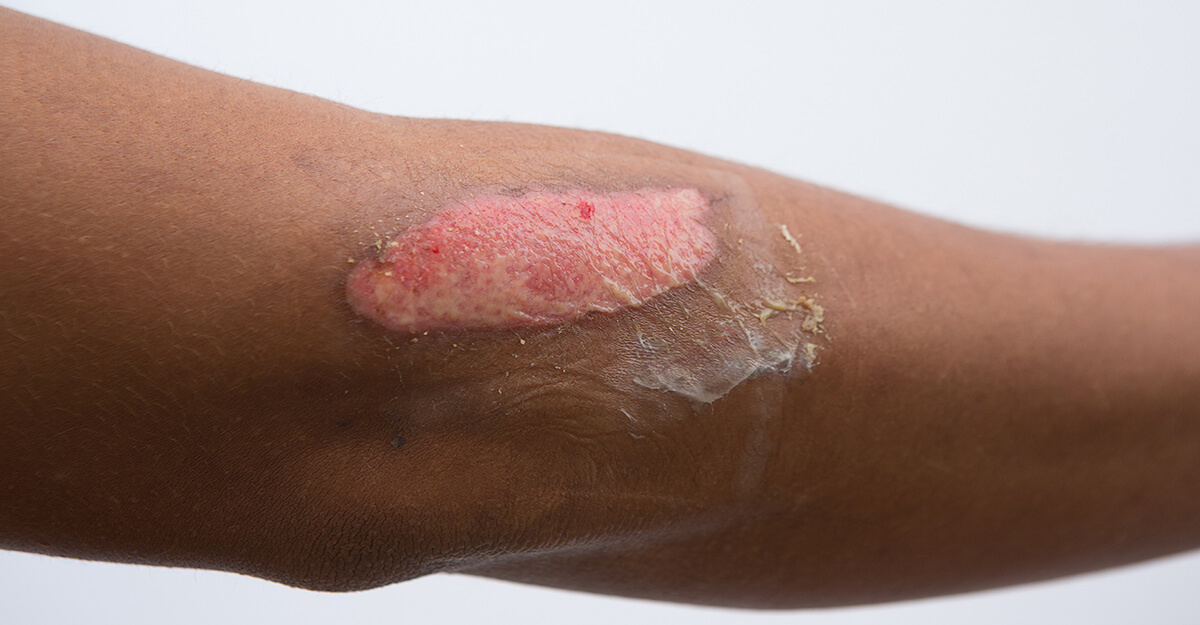
Damage extends through the epidermis downward into the papillary or superficial into the dermal layer. Dermal structures are intact such as nails, hair follicles, nerve endings, and sweat glands. Characterized by large blisters, edema, and pain. A wet, weeping, shiny surface can lead to permanent scarring and may need to be grafted. The patient may experience extreme pain since the wound leaves nerve endings exposed. Common causes include contact with flash injury, flame injury, and scalding liquids.
Deep partial thickness (deep second degree)
The burn extends deeply into the reticular layer of dermis and can quickly evolve into a full thickness burn. Skin will typically be splotchy red or waxen and white, wet, and not form blisters. Depending on how much nerve damage has taken place, deep partial-thickness burns can be relatively painless.
Full thickness (third and fourth degree)
The burn extends into the subcutaneous tissue or further into muscle, bone, and tendon (fourth degree). Characterized by deep red, black, or white appearance, edema present, painless nerve ending damage, and exposed subcutaneous fat layer. Grafting is necessary. Common causes include prolonged flame (such as in a house fire), steam or scalding liquids, and chemical or electrical injury.
Despite the revised terminology, many clinicians and burn centers still use a combination of both forms.
What Causes Burns?
Let’s go through a quick list of types of burns and what can cause them:
- Friction burns are produced by contact with a surface that rubs off the skin like in a carpet burn.
- Thermal burns involve either cold or heat.
- Cold burns are frostbite injuries and heat-related burns are caused by flame injury, hot metal, and scalding liquids.
- Radiation burns include tissue damage as a result of sunlight or x-rays/radiation therapy.
- Chemical burns are created by contact, ingestion, injection, or inhalation of strong acids or alkaline substances.
- Electrical burns involve contact with faulty or exposed electrical wiring or high voltage power lines.
How to Treat Burn Wounds
Treatment is determined by the cause, severity, and characteristics of the wound and impact on function and mobility. The basic principles of promoting moist wound healing, cleaning the wounds of debris and necrosis, and managing the bioburden risk are similar to other wounds.
Unfortunately, there are many dressings that are contraindicated for use as a primary dressing. Therefore, it is imperative that clinicians read the manufacturer insert regarding for what wounds the product is indicated and contraindicated.
When dealing with superficial and partial thickness burns, debridement is rarely needed, and the focus is on keeping the wound moist and controlling or preventing bioburden issues.
Full thickness burns often require debridement initially, such as sharp or mechanical, to remove the necrosis and debris. It also contributes to reducing bacteria that can lead to infection. Due to the higher risk of infection with both partial and full thickness burns, topical antimicrobial agents are often employed and are more effective than systemic antibiotics since they are unable to be delivered to the damaged tissue. Common agents such as Silvadene, Sulfamylon, Bacitracin, and Anasept are used effectively to manage the bioburden.
In cases where burns cross the joints of the body, patients will often undergo extensive therapy to increase or maintain range of motion along with splinting or positioning to prevent contractures and the loss of mobility and function.
Finally, the implementation of pressure may be needed to reduce edema and/or hypertrophic scarring.
The American Burn Association has developed specific guidelines for referral of a burn patient to a burn center, as most small or general hospitals are not equipped to deal with extensive and severe burn cases. You can find this and lots of additional helpful information at www.ameriburn.org.
Take our engaging, evidence-based Wound Care Certification Courses for nurse, registered dietitians, physical therapists, and more professionals. Choose the format that suits you and get access to tools to help you ace your exam.
What do you think?