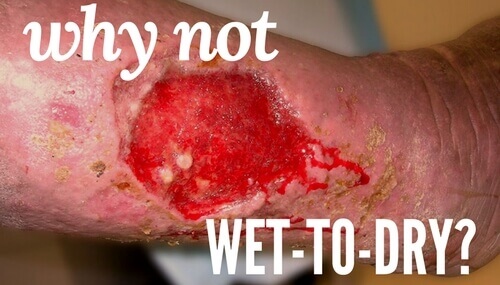
What should wound care professionals do when a physician orders wet-to-dry dressings? Be prepared and know the facts.
Those of us in wound care know that wet-to-dry dressings are considered substandard care. Some physicians, however, commonly order wet-to-dry dressings for patients, often leaving clinicians in a tricky situation. Do you feel conflicted as to how you should respond? It can be intimidating, but with a little preparation, it doesn’t have to be. By knowing the facts about wet-to-dry dressings, as well as effective and cost-efficient alternatives, you can handle such situations with confidence. Not sure where to start? We’re here to help.
What are Wet to Dry Dressings?
Wet-to-dry dressings are a non-selective form of mechanical debridement, which is a method of removing non-viable tissue from the wound.
Dressing steps
- The wet-to-dry technique begins when the clinician applies gauze (moistened with sterile saline or water) to the wound bed.
- The dressing is allowed to dry and adhere to the tissue in the wound bed.
- Every four to six hours, the clinician firmly pulls the dry gauze (not re-moistened) from wound bed at a 90-degree angle. This also pulls the adhered tissue – both viable and non-viable – from the wound.
The Downside
The wet-to-dry technique comes with clear disadvantages:
- As a non-selective method, it often removes healthy tissues.
- The re-injury of tissue causes bleeding and pain for the patient.
- It can leave strands of gauze behind in the wound bed. Foreign bodies in the wound can lead to granuloma formation and/or infection.
- Local tissue cooling during the evaporation period causes vasoconstriction (narrowing of blood vessels) and hypoxia (deficiency in the amount of oxygen reaching the tissues). This will impede the wound-healing and increase the susceptibility to infection.
- The removal of a dry dressing may serve as an airborne vector for bacteria.
The drawbacks above apply even when wet-to-dry is used as intended, during the inflammatory phase of wound healing. Unfortunately, wet-to-dry techniques are often used improperly over granulation and epithelialization tissues in the proliferative phase, which disturbs collagen deposition, angiogenesis (the in-growth of blood vessels) and re-epithelization. This slows down healing and increases the risk of soft tissue infection and osteomyelitis.
Wet-To-Dry Alternatives
Once you raise your fact-based concerns about wet-to-dry dressings, follow-up with solutions in the form of effective and cost-efficient alternatives.
Debridement
In another post we dove further into the following debridement types:
- The selective methods – autolytic, enzymatic, and biological – remove only the non-viable tissue and are much less painful for the patient while also promoting healing.
- The non-selective methods – mechanical and sharp – can also be useful, though they can remove healthy tissue. For example, consider using sharp debridement when there is a question of underlying infection.
Remember, though, that all forms of debridement should be used only during the inflammatory phase of wound healing.
Dressings
In the days when wet-to-dry was part of standard medical education, we didn’t have the same options we have today. Gauze was king, and widely considered to be the most cost-effective option – even as new dressings were being developed. However, gauze dressings require frequent changes and are less effective in maintaining an optimal warm and moist healing environment.
Today’s dressings can insulate the wound, donate moisture, protect from bacterial invasion, and absorb high levels of exudate or stimulate tissue development as needed. Many dressings even promote autolytic debridement. By allowing longer wear times, reducing infections, and promoting more rapid wound healing, these dressings can cost less than gauze over time.
Free Wet-To-Dry Dressing Webinar
Are you ready to find out more about wet-to-dry dressings and their more effective alternatives? WCEI instructor Don Wollheim, MD, FAPWCA, WCC, DWC, is a Wound Care Certified surgeon who completed medical school when wet-to-dry was the standard. He understands why some physicians resist the shift in thinking. In his webinar, he arms you with the knowledge you need to counter this resistance. View the one-hour webinar “Wet-to-Dry Dressing: The Good, the Bad, the Options” for free with the coupon code BLOG (education credit available).
Want to learn more about Skin & Wound Care?
Get Started →What do you think?