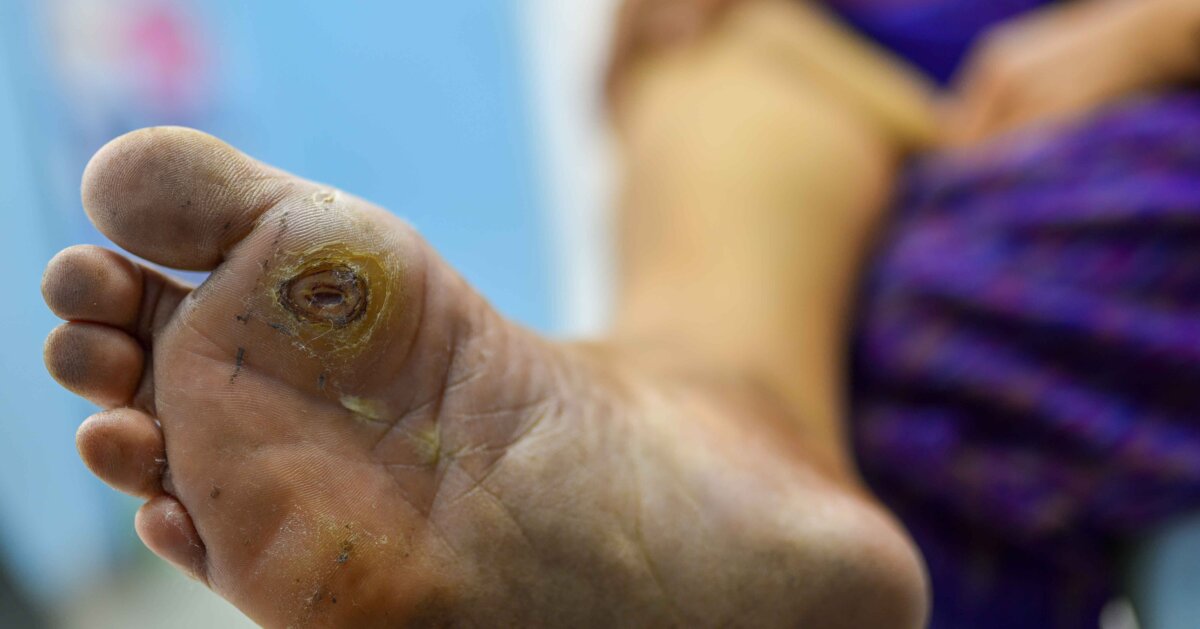
Diabetes wounds can be some of the most challenging to treat, even for the most experienced wound care professionals. As the prevalence of diabetes continues to grow, with 38% of U.S. adults having prediabetes, whether you are new to wound care or a seasoned professional, you will most likely encounter patients with diabetes on an increasing basis.
The American Diabetes Association recognizes November as American Diabetes Month, and as of 2022, diabetes has affected 37.3 million people in the United States. Having diabetes can complicate and delay the healing process of any type of wound, including pressure injuries, venous ulcers, arterial ulcers, or trauma wounds.
However, diabetes wounds can be especially pervasive, as they are known to be slow to heal, and there are numerous reasons why. One reason is that the cells most responsible for healing cannot correctly function when the patient has elevated blood sugars or has developed hyperglycemia with an increased risk for arterial disease.
These complications can result in smooth muscle cell dysfunction, fibroblasts being unable to efficiently build new collagen structures, and phagocytic cells being unable to remove bacteria and create cytokines and growth factors, which is needed for effective wound healing.
Diabetes wounds can affect different regions of the body; however, diabetic foot ulcers (DFUs) are the most common wounds sustained by diabetic patients. These ulcers typically occur below the ankle, and 85% of amputations of the foot are preceded by this type of ulcer. And, unfortunately, recurrence rates for DFUs are high with 40% of patients experiencing a recurrence within one year.
Types of ulcers
DFUs can occur on patients with either type 1 or type 2 diabetes and can vary in severity. These ulcers are identified differently based on certain symptoms presented. Knowing and understanding the differences can help in determining the correct treatments.
- Neuropathic: Neuropathy causes a loss of sensation, movement, or autonomic function in a specific part of the body. A patient has a neuropathic ulcer when they experience a lost sensation but do not have underlying arterial disease. According to one study, up to 50% of individuals with diabetes will experience neuropathic ulcers in their lifetime.
- Ischemic: Ischemia is when oxygen and blood flow are restricted or reduced in a certain area. When ischemia is present, but sensation is not yet lost, the ulcer is ischemic. Arterial disease can be present as well, and this condition affects over 50% of diabetic patients. The risk of peripheral artery disease increases by 26% for every 1% rise in the A1C level.
- Neuro-ischemic: An ulcer is neuro-ischemic when both neuropathy and ischemia are present. This sub-type makes up nearly 50% of DFUs.
While there are differences in ulcer types, they share similarities in how they occur. DFUs arise primarily from neuropathy, vascular disease (with associated ischemia), or both, and are often complicated by an infection/biofilm. Contributing factors include limited joint mobility, callus formation, high foot pressures, and increasing susceptibility to ulceration. DFUs are complicated with multiple components, and you must be very observant. By using multiple interventions and approaches, you can achieve successful wound healing.
7 essential steps for healing
Step 1: Remove the cause of the wound. Eliminating the cause of the wound is crucial. While diabetic patients may have other conditions that factor into the occurrence of DFUs, these ulcers can often be caused by ill-fitting shoes or trauma related to the foot. Removing the cause of the DFU will help with wound healing and aid in the maintenance of keeping the wound closed after it has healed. If a patient is put back in a shoe that caused the DFU, the wound may reoccur.
Step 2: Create and maintain a moist wound environment. Wounds heal best in a moist environment. There is faster granulation, angiogenesis, and re-epithelialization. Monitor for infection, as bacteria also grows best in a warm, moist environment. Dressing selection must foster the removal of biofilm, control bacteria, encourage debridement if necessary, and facilitate an environment where a wound can granulate and re-epithelialize.
Step 3: Remove any necrotic tissue (slough or eschar) and calluses. Callus formation is a sign of friction or rubbing. Callus build up is often a first sign of an ulcer in a diabetic patient. When a callus is present, it needs to be debrided — often with serial debridements. Necrotic tissue serves as a reservoir for bacteria to grow, so it is vital to remove this as quickly as possible.
Step 4: Effectively manage the bioburden, infection, and biofilm. Management of bacteria is essential since DFUs often struggle with bacterial growth, infections, and biofilms. Diabetic patients tend to have muted inflammatory responses, so treating them aggressively with topical antimicrobial cleansers and antimicrobial dressings is key. Quick removal of dead or necrotic tissue from the wound bed will also help to manage bacteria.
Because diabetic patients often have compromised immune systems, more frequent monitoring of these wounds is necessary during the inflammatory phase, and early prevention of biofilms can also enhance wound healing. In addition, techniques such as effective cleansing with each dressing change using an antimicrobial cleanser, removal of necrotic tissue, and the use of antimicrobial dressings can help reduce the use of systemic antibiotics. For this type of wound care, you must be cognizant of the diabetic patient and how hyperglycemia can interfere with all phases of healing.
Step 5: Ensure adequate tissue perfusion. Adequate blood flow to the wound bed is essential in patients with DFUs. Giving an ankle-brachial index (ABI) test early on with any lower extremity wound, along with a comprehensive foot exam, can help determine if a referral to a vascular specialist is needed. In these situations, early intervention is key.
Patients with compromised arterial blood flow may need surgical revascularization to get adequate blood flow, specifically the RBCs carrying oxygen to the wound bed, so that healing can take place. Other non-surgical interventions, including prescribed medications like anti-platelet medications, statins, and ACE inhibitors (which have been shown to improve circulation) can also be considered. For patients with type 2 diabetes, clinical evidence supports the use of statins and ACE inhibitors for both management and prevention of cardiovascular health.
Step 6: Encourage and provide patient education on healthy nutrition. Adequate nutrition, ensuring metabolic demands are met, and the control of blood sugars are vital for diabetic wound care. All DFU patients need protein for all phases of wound healing, and protein is key for important fibroblasts to build new collagen structures. Other important components to facilitate wound healing are calories via carbohydrates and fats, as well as vitamins and essential amino acids. Diabetic patients can consult with a dietician to ensure their nutritional needs and goals are being met.
It is also important to monitor blood glucose levels and ensure they stay lower, as this helps cells working at the wound bed to be more productive. To keep blood glucose levels down, some patients may need sliding-scale insulin and/or insulin supplementation — especially during times of stress or infection.
Step 7: Off-loading of all DFUs. Off-loading methods are beneficial for the treatment of plantar surface DFUs. Redistributing pressure off the plantar surface, or complete off-loading of a DFU, has shown to exponentially increase healing times. Effective off-loading can occur with equipment such as wheelchairs and crutches; however, total contact casts are considered the “gold standard” of treatment for off-loading foot ulcers.
Do not overlook adjunctive treatments
If the wound does not respond within 30 days after following the steps above, consider the use of adjunctive treatments, such as hyperbaric oxygen therapy, negative pressure, grafting, additional off-loading, ultrasound, e-stimulation, or Regranex (a topical medication).
It is also helpful to get a second opinion for non-healing wounds, keeping in mind that inadequate blood supply to the wound, elevated blood sugars, and/or insufficient protein intake can disrupt the healing process. Patients with DFUs are typically monitored more closely, receiving comprehensive evaluations and follow-up appointments, which include measurements to monitor the wound’s healing. Based on the changing quality of the ulcer, treatment strategies can be modified.
Recognizing the cause of the wound with quick and effective wound care interventions can ensure faster healing times. Education on DFUs and other diabetes wounds is key for the successful treatment and prevention of further ulcers in diabetic patients.
Editor’s Note: This post was originally published in March 2019 and has been updated with new content.
Take our engaging, evidence-based Wound Care Certification Courses for nurses, registered dietitians, physical therapists, and more professionals. Choose the format that suits you and get access to tools to help you ace your exam.
Learn MoreWhat do you think?