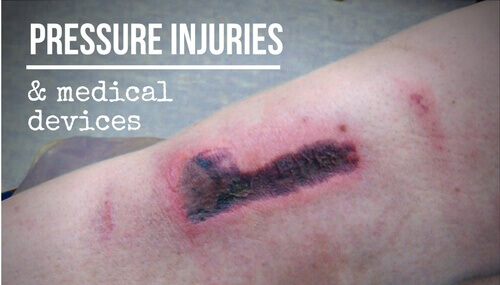
Medical device-related pressure injuries (MDRPIs) are a standard part of wound care, but preventative practices can make a big difference.
One of the first things clinicians learn about treating pressure injuries is to find the cause of the pressure and simply remove it. Sounds simple, doesn’t it? But what do you do when the cause of the pressure injury is a medical device which is not only necessary, but literally sustaining a patient’s life?
While some medical device-related pressure injuries are unavoidable, there are things clinicians can do to relieve the pressure and heal the injury. Here’s what you need to know.
What Are Medical Device-Related Pressure Injuries?
A medical device–related pressure injury (MDRPI) is a localized injury to the skin or underlying tissue resulting from sustained pressure caused by a medical device. The most common medical devices that cause such pressure injuries are:
- braces
- splints
- casts
- respiratory masks or tubing
- tracheostomy tubes
- collars or straps
- feeding tubes
- negative-pressure wound therapy devices
The dilemma is in finding a way to relieve the pressure and heal the wound without having the option of device removal. So then, what can you do?
It’s All About Prevention
While there are some medical device-related pressure injuries that just aren’t avoidable, there are preventative practices you can put in place to avoid them. For instance:
- to avoid pressure injuries caused by a poorly positioned or secured device, frequently evaluate device positioning and securement.
- to avoid pressure injuries under the tubing or device, loosen the device at least once per shift to check for skin problems.
MDRPI Resources Are Available
Thanks to the National Pressure Ulcer Advisory Panel, there are a number of educational resources available that can serve as meaningful guides for treating MDRPIs. They include four helpful Best Practices for Prevention of Medical Device–Related Pressure Injuries posters. The series includes one for: general best practices; critical care; pediatrics; and long-term care.
Each poster features photos of MDRPIs and prevention strategies, such as how to:
- choose the correctly-sized medical device for the individual.
- cushion and protect the skin with dressings in high-risk areas.
- remove or move the device daily to assess skin.
- avoid placing the device over the site of a previous or existing pressure ulcer.
- educate staff on the correct use of devices and prevention of skin breakdown.
- be aware of edema under the device and the potential for skin breakdown.
- confirm that the device isn’t placed directly under a bedridden or immobile patient.
While prevention can go a long way in avoiding MDRPIs, that doesn’t mean they won’t happen. For as long as patients need medical devices, related pressure injuries will occur. Even though some of them are unavoidable, clinicians and caregivers can make a difference.
We can focus on prevention and learn from our mistakes or experiences. We can determine the cause of the MDRPI and minimize risk. And we can take steps to heal our patients while preventing future pressure injuries as best we can.
What Are Your MDRPI Experiences?
Do you have any advice to give others for treating patients with MDRPI? Have you implemented preventative practices that have made a difference, or are there specific patient stories about this topic you can share? We’d love to hear about them – please leave your comments below.
Wound Care Education Institute® provides online and onsite courses in the fields of Skin, Wound, Diabetic and Ostomy Management. Health care professionals who meet the eligibility requirements may sit for the prestigious WCC®, DWC® and OMS national board certification examinations through the National Alliance of Wound Care and Ostomy® (NAWCO®). For more information see wcei.net.
What do you think?