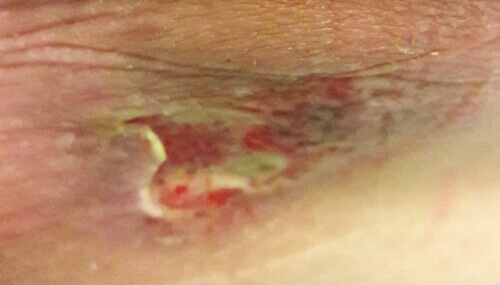
Trained wound care clinicians truly make a difference in the lives of their patients. This caregiver knows first-hand, and wanted to share her story.
Recently, a 45-year-old caregiver by the name of Annie* contacted WCEI for help. She was desperate and in search of answers. Her personal account serves as a sobering reminder of why we do what we do. Here is her story.
The Challenges of Caregiving
Since 1995, Annie has been the primary caregiver for her mother, Helen*, who has Multiple Sclerosis. Helen is wheelchair bound, but lives an active life, attends church and other social gatherings, spends time outdoors and enjoys shopping.
Through good days and bad, Annie is by Helen’s side. “I’m determined to do an amazing job taking care of my mother,” says Annie. “So that when my nieces and nephews ask me, ‘How is Grandma?” I can say she’s doing well, and they’ll know that I’m doing the best I can.”
An Unexpected Problem
If there’s one thing Annie has, it’s patience; there are rarely quick fixes to the health complications that her mother’s condition brings. But last December, Helen developed a sacral pressure injury, and it would prove to be one of the biggest tests of her patience so far.
The family’s home care nurse first diagnosed the pressure injury as “Stage 1/Stage 2” during a regular weekly visit, dressed it, and left behind additional dressings for the week. The next day, the wound showed improvement, so Annie was hopeful.
When the nurse visited the following week, however, she brought with her a different type of dressing. Soon the wound yellowed, was dry and looked like a spider web. “I called the nurse immediately, but she wasn’t really responsive,” said Annie. “She didn’t seem to be concerned, and the next day it started to turn mushy, was deeper and started to smell.”
By the time the nurse came back for a third weekly visit, the wound was at a “Stage 3/Stage 4.” Annie was told to offload her mom (without detailed instructions), and so she did her best, but flash forward to the end of January, and:
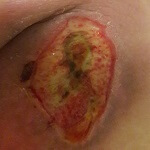
January 30, 2017
- Helen’s wound had been treated with a total of three different types of dressings.
- Annie was left feeling confused and frustrated by vague instructions and what she viewed as unresponsive clinicians.
- The pressure injury had doubled in size, and was still mushy, yellow and showing no signs of improvement.
Desperation Sets In
“At that point, I’d had enough,” Annie said. “I kept taking pictures of the wound, but I didn’t know what was going on. It was disgusting – it smelled so bad, and nothing was working. I just stopped putting anything on it at all.”
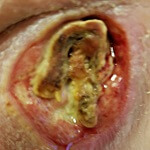
February 15, 2017
The nurse was dumbfounded and clearly didn’t know what to do. Annie started conducting research on her own and learned that silver-based dressings help with infection. Upon reflection, she realized that the very first dressings used for the pressure injury were that type, but unfortunately, they were never used again. When Annie addressed this with the nurse, she was told that those original dressings were too costly, and that, “They’re are all the same anyway.”
Annie took it upon herself to keep digging, and read that colloidal silver helps to dry wounds. “I bought a bottle of it for $40, and the wound dried up and smelled better, but I knew it wouldn’t heal the pressure injury,” she said. “That’s when I reached the end of my rope and called WCEI.”
A Call for Help
When Annie decided to contact us, she had not only spent countless hours scouring the internet for answers, she had also reached out to additional local resources in search of help. This included visiting a wound care clinic, but she found the staff to be unresponsive, and left the facility without clear direction or a plan of action.
“Until I called WCEI, I felt like no one understood,” said Annie. “I was trying hard to stay calm, but I felt so angry and bitter … I know the nurse and other clinicians were doing their jobs the best they could, but they simply didn’t know what to do. And I’m the one that had to deal with the consequences. I assumed that every nurse would know how to treat a wound. But now I know that’s not the case.”
Annie then got in touch with a different home health agency, and found a nurse that could come visit Helen (and bring appropriate dressings). She has also learned how dehydration can deter healing, and how a moist wound environment, coupled with the right dressings at the right time, can make all the difference.
Annie has encouraged agencies to send their staff to WCEI events, and has become an advocate for caregivers and proper wound care. She is even planning on attending a one-day WCEI seminar so she can increase her own wound care knowledge.
A Happy Ending
Today, after almost three months since Helen’s pressure injury was first diagnosed, the wound is finally getting better, and there is no infection.
“In all the years I’ve been taking care of my mother, nothing has been more stressful than dealing with this wound,” Annie said. “Seeing her in pain has kept me up at night and in tears. She’s a tough lady, but she already has limitations to deal with, and this was an added burden.”
Annie said that from her personal experience, she’d like to see more awareness of what home-bound patients need so they can get the same care as those in facilities. “As a caregiver, I just wanted to be taken seriously. And my journey in wound care was made harder because of the lack of knowledge on the clinicians’ parts. That extra knowledge would have made such a big difference in this experience.”
What Do You Think?
We were touched by Annie’s story, and know that it serves as a reminder about the importance of educated wound care professionals. We’d love to hear your feedback. Have you heard similar stories from caregivers or patients? Have you been in the position to help a patient recover from negligent wound care? Please share your stories and comments below.
*Names have been changed to protect the privacy of those involved.
Wound Care Education Institute® provides online and onsite courses in the fields of Skin and Wound, Diabetic and Ostomy Management. Health care professionals who meet the eligibility requirements may sit for the prestigious WCC®, DWC® and OMS national board certification examinations through the National Alliance of Wound Care and Ostomy® (NAWCO®). For more information see wcei.net.
What do you think?