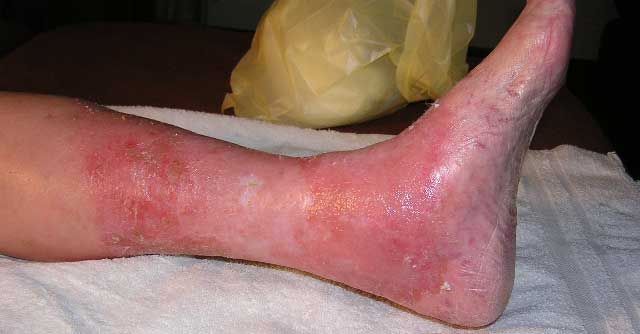
In my experience, I have encountered the confusion between venous dermatitis and cellulitis that plagues the wound care industry.
The unlikely diagnosis of “bilateral cellulitis” is not uncommon in wound care, followed by two weeks of unnecessary antibiotic therapy.
Despite some similarities, there are many differentiating characteristics that diagnosing clinicians either overlook or misunderstand.
In an effort to help clinicians more accurately differentiate the two conditions, we will discuss the differences in this blog post. It will help you prescribe appropriate treatments and improve patient outcomes.
What is Stasis Dermatitis?
Stasis dermatitis, which is also known as venous stasis dermatitis, venous eczema and gravitational dermatitis, is a common condition that develops early in patients with venous insufficiency.
The valvular damage that occurs and then leads to venous hypertension and edema set the stage for stasis dermatitis.
There are several theories that lead to the cutaneous inflammation in patients with venous disease, including Hypoxia/stasis and Fibrin cuffs, according to an article by Scott L. Flugman.
A patient’s prior history often includes hemosiderin staining, pruritis, medial ankle involvement and edema.
The physical examination of the lower legs reveals patches of erythematous, eczematous and/or scaling, itching skin.
As the problem advances, the inflammation can encircle the ankle and extend to just below the knee. In more severe and acute cases, exudative or weeping patches and plaquescan exist, according to an overview by Medscape.com.
With the chronicity of venous insufficiency and stasis dermatitis, lichenification and hyperpigmentation can manifest because of chronic scratching.
The skin can become indurated and progress to lipodermatosclerosis, as well as develop plaques and nodules on the legs and dorsal foot. These conditions will most often present bilaterally, not unilaterally.

Stasis Dermatitis Treatment Options
Diagnostically, blood tests are generally not helpful unless cellulitis is also suspected. Doppler studies in patients with acute new onset of stasis dermatitis can be a prudent option to rule out thrombosis or severe valve damage.
In rare circumstances, skin biopsies are taken in acute or subacute conditions. However, biopsy could be necessary in chronic dermatitis if acroangiodermatitis has developed.
Treatment is a multi-faceted approach that starts with therapeutic level compression (30-50mmHG), along with effective calf pump activation via weight-bearing activities such as walking and standing calf exercises.
Frequent elevation of the legs throughout the day can be helpful and necessary if patients are not activating their calf muscle pumps sufficiently or wearing appropriate levels of compression.
With chronic venous disease, treatment of the lymphatic system with Complete Decongestive Therapy (CDT) may be beneficial or necessary.
Topical approaches are similar to other forms of acute eczematous dermatitis, including drying agents (i.e. aluminum acetate) with weeping lesions and corticosteroids to reduce the inflammation and itching.
Long-term management of stasis dermatitis focuses on treating the venous disease and good skin care.
What is Cellulitis?
By contrast, cellulitis is a non-necrotizing inflammation of the skin and subcutaneous tissue, typically from acute infection after a break in the skin.
The sudden onset is marked by signs of erythema — which increases as infection spreads — warmth, pain and swelling. The borders of the involved area are not sharply demarcated or elevated. With uncomplicated cases involving only limited area, minimal pain, no systemic symptoms and no serious risk factors, there is no workup.
Blood cultures, CBC with differential, creatinine, bicarbonate, creatine phosphokinase and C-reactive protein levels should be assessed with symptoms of systemic involvement per the CDC. Streptococcal bacteria are the most typical cause, followed by staphylococcal.
Treatment will consist primarily of antibiotic therapy. If abscesses exist, they will need to be drained appropriately. Infectious disease may need to be consulted if the condition is not improving with standard treatment, or if an unusual organism is identified.
Elevation of the extremity can reduce swelling, and warm compresses to the involved area can increase blood flow to bring more of the body’s own anti-inflammatory cells to the site to fight the infection.
Despite some misunderstandings or misinformation currently perpetuated, compression is actually beneficial and recommended to assist in maximizing venous flow, lymphatic uptake and stimulation of the lymphatic system, thus improving immune system function.
As with any wound or medical condition, we must always remember the most important part — diagnose, diagnose, diagnose.
Take our course on Skin and Wound Management.
What do you think?