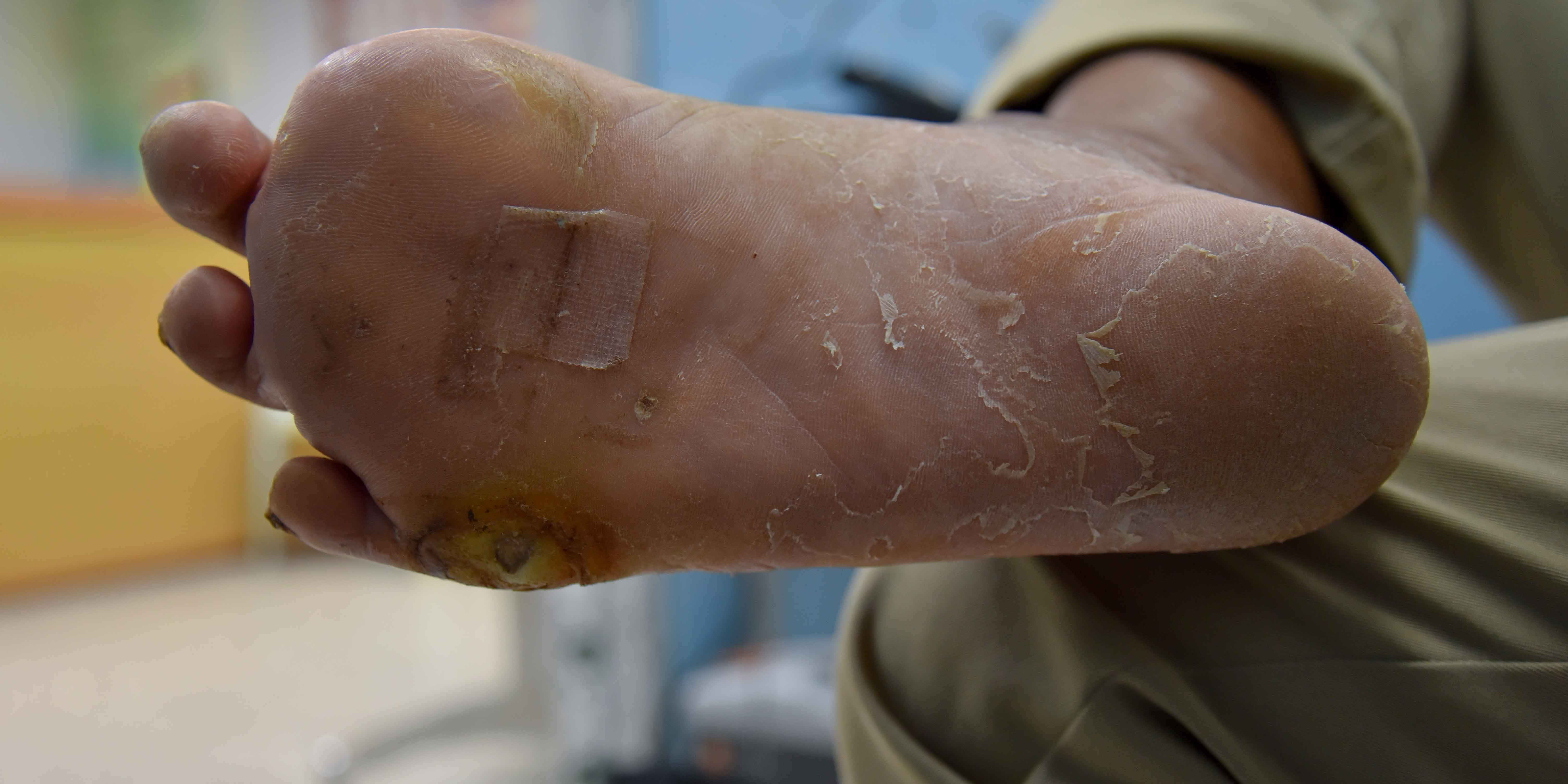
With more than 30 million people in the U.S. afflicted with diabetes, clinicians are very likely to encounter diabetic patients.

By Carole Jakucs, MSN, RN, PHN
Diabetic foot ulcers occur in approximately 15% of diabetic patients. And if you’re a wound care clinician, you’ll likely find yourself caring for patients with diabetic foot ulcers more often than not.
To learn more about the causes and how to prevent diabetic foot ulcers, we spoke with Don Wollheim, MD, FAPWCA, WCC, DWC, a board-certified surgeon of the American Board of Surgery.
He has 25 years of experience in general/vascular surgery and 13 years of experience as a wound care specialist and educator. Wollheim is also a medical-legal consultant, college science instructor and clinical instructor at the Wound Care Education Institute (WCEI).
Wollheim said there are three important facts to know about diabetic foot ulcers:
- They can be prevented.
- They are the cause of 85% of the amputations in diabetic patients.
- There are 225 amputations related to diabetic foot ulcers performed in the U.S. every day and amputations every 30 seconds worldwide.
Given these astounding realities about diabetic foot ulcers, it behooves patients and the clinicians caring for them to understand what causes diabetic foot ulcers.
Actively engaging in effective prevention strategies can help reduce the risk of developing diabetic foot ulcers and the life-altering complications that can ensue.
Causes of diabetic foot ulcers
To understand the pathophysiology of diabetic foot ulcers, it’s essential to know the three different types that can occur, Wollheim said.
The types include:
- Ischemic
- Neuroischemic
- Neuropathic
Ischemic ulcers occur because of an underlying vascular problem and tend to happen more often in the toes and the lateral aspect of the foot.
With neuropathic foot ulcers, patients have lost some degree of sensation, making them susceptible to injuries they cannot feel and have no awareness of. Neuropathic wounds generally occur on the plantar/walking aspect of the foot.
Diabetic foot ulcers that are neuroischemic are caused by a blend of two factors being present in patients — neuropathy as a result of diabetes and peripheral artery disease.
Wollheim said peripheral neuropathy occurs as a result of high blood glucose levels and affects the nerves going into and out of the feet. There are three different types of nerves that are injured:
- Peripheral sensory: 75% experience a numb foot and 25% of these patients experience pain as a result.
- Peripheral motor: This stems from the nerves coming from the spinal cord and affects the innervation and muscle tone of the foot.
- Peripheral autonomic: This condition affects various involuntary body functions and organ systems but also presents with integumentary symptoms such as dry and cracked skin.
Prevention of diabetic foot ulcers
It’s important for clinicians to focus on diabetic foot ulcer prevention.
“If we can prevent diabetic foot ulcers from occurring in the first place, we can prevent a whole lot of amputations in these patients,” Wollheim said.
Ways to prevent diabetic foot ulcers involve both patients and clinicians, with patients needing to practice continuous self-care while following the important advice of their clinicians, Wollheim said.
More than a dozen pertinent prevention strategies include:
- Weight control: Encourage patients to maintain a normal weight for their height to help prevent the development of insulin resistance and type 2 diabetes.
- Early diagnosis of diabetes: Get a handle on out of range/high blood glucose, sooner, rather than after nerve damage has occurred.
- Healthy levels: Strive for good glucose control and an A1C level lower than 7%.
- Stay connected: Advise patients on the importance of following up with their clinicians as requested for ongoing skin and foot surveillance and timely medical treatments should wounds occur.
- Care path: Clinicians should follow the recommendations of the American Diabetes Association regarding foot exam frequency and adhering to the exam schedule as per each of the four risk categories (0,1,2,3).
- Stay covered: Always wear socks and shoes to help keep feet clean and dry, protect feet from injuries and decrease friction and shearing. These occur by wearing shoes without socks.
- Changes are good: Change shoes at least once a day to prevent ongoing friction in the same spots of the feet for prolonged periods of time from the same shoes.
- Time of day matters: When purchasing new shoes, do so in the afternoon or early evening when feet are usually at their largest size.
- Find a good fit: Shoes need to accommodate the feet. Don’t expect feet to adapt to the shoes. Poorly fitted shoes can cause foot trauma.
- Style choice: Stay away from loafer styles and go for shoes with ties or Velcro for more flexibility.
- Break in shoes: Before taking them on vacation, test new shoes since extra walking typically occurs on vacation when sightseeing.
- Protect yourself: Don’t go barefoot. It’s too high a risk of skin/foot trauma.
- Set a daily habit: Practice daily self-foot exams and seek care the same day for any redness, swelling, callouses, blistering, increased warmth, laceration, lesion or deformities.
- Don’t self-treat: Avoid self-treating callous or other wounds. All wounds need to be treated correctly by a wound care specialist to prevent them from becoming a diabetic foot ulcer.
- Look for deformities: Fractures can occur without patients knowing it if they cannot feel pain.
- Custom fit: Patients can consider purchasing custom-made shoes if foot deformities are already present, such as hammer toes and bunions.
- Trust your eyes: Inspect all aspects of the foot with daily foot exams, including the bottoms of the feet and between the toes. Enlist the use of mirrors as needed to see the whole foot.
- For patients with neuropathy: If taking tub baths, check bath water with a thermometer before dipping the toes and feet in water that’s too hot. This will help prevent burns.
Learn more in our Diabetic Skin and Wound Management course.
What do you think?