Key Takeaways
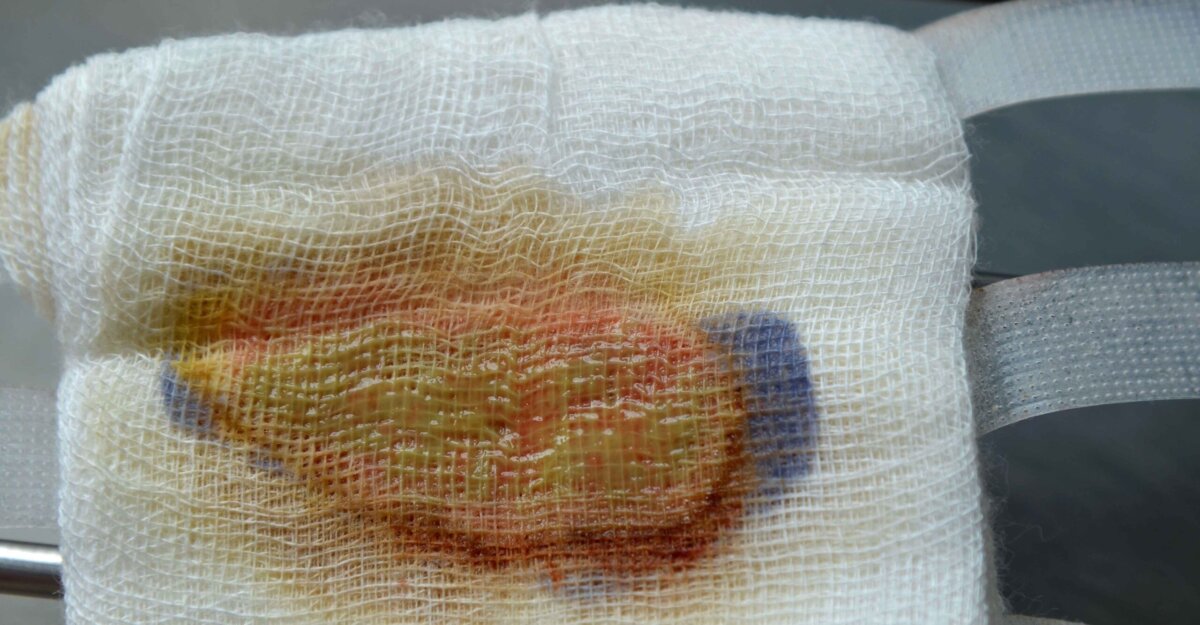
Purulent drainage, characterized by its thick, milky consistency and foul odor, indicates a potentially serious wound infection and requires prompt assessment and treatment, typically involving antibiotics and specialized wound care techniques. Early recognition and intervention are crucial to prevent the infection from advancing to more severe stages that could lead to systemic issues. Monitoring wound signs and symptoms, along with potential specialist referrals, are vital for effective management and healing.
Whether you call it drainage or exudate, it is important to understand the different types of fluid, especially when it appears more severe. Purulent drainage is considered the most serious type of exudate, so recognizing what to look for and how to treat it can help wounds heal more effectively.
Each drainage type — serous, sanguineous, serosanguineous, seropurulent, and purulent —varies in quantity, color, consistency, and odor. The consistency can range from thin and watery to thick and gelatinous, and the color may be clear, yellow, pink, red, green, opaque, or tan.
Normal wound exudate is often clear, yellow, pink, and red. However, significant red drainage may require a closer look, as the wound may have active and ongoing bleeding. And green is likely a sign of pseudomonas infection and is usually accompanied by an odor.
Purulent is deemed the most severe exudate type. Appearing tan, opaque, or milky in color, this exudate can be a sign of increasing wound colonization or infection. Here, we take a closer look at purulent drainage, noting characteristics, causes, treatments, and challenges.
What is purulent drainage?
The National Institute of Health defines purulent drainage as “pus containing fluid that is draining from an orifice or wound.” It may be milky, gray, brown, or yellow and is typically thick in consistency with a foul odor.
Consisting of bacteria, white blood cells, and wound debris, this exudate can also be found in chronic wounds such as pressure injuries and diabetic foot ulcers. You may also see this type of drainage in acute wounds such as trauma injuries and surgical incisions.
Purulent drainage causes
When purulent drainage is present, it is a sign the wound is unhealthy and may be infected. Impaired wound healing will accompany this drainage type, so it is imperative to identify and report it.
It’s important to note that the presence of odor alone does not indicate infection. Mild odor may be noted in chronically colonized wounds. Thoroughly cleansing the wound and disposing of the soiled dressing should rid the wound of odor. If the wound remains malodorous after following these steps, infection is likely.
Difficult-to-treat wounds such as pressure injuries, arterial ulcers, and diabetic foot ulcers are at an increased risk for infection due to their chronicity. Patients with diabetes, impaired vasculature, malnutrition, and obesity are susceptible to wound infection. People who smoke, patients who are being treated for active cancer, and older adults are also at risk.
If you’re looking to gain a more in-depth knowledge of how to provide advanced skin & wound care, our Skin and Wound Management courses can help.
How to treat purulent drainage
To treat purulent drainage, it is necessary to first assess the wound for other signs of infection. An oral antibiotic will likely be the first line of treatment. But the clinician may want to culture the wound to help guide antibiotic treatment. It is important to thoroughly cleanse the wound prior to obtaining a culture, which should be obtained from exposed wound tissue being careful to avoid necrotic tissue and drainage as much as possible.
When obtaining a wound culture, the Levine technique is typically preferred over the Z technique. The Levine technique helps to express drainage from the wound bed itself, thereby providing a sample from both the wound bed and just below the surface. The Levine technique is done by rotating the culture swab over a small area of the wound bed using mild pressure.
Treating purulent drainage also includes managing the drainage caused by the infection. This is vital, as copious, unmanaged drainage will macerate and breakdown the intact peri-wound skin. Choosing wicking dressings (e.g., alginates and hydrofibers) as primary dressings and absorptive secondary dressings (e.g., foams and superabsorbers) will help with drainage control.
Clinicians may choose to use silver impregnated dressings for their antimicrobial benefit. And hypochlorite or acetic acid cleansings and soaks may be used to help control the bacterial burden of infected wounds.
The challenges
The most common challenge is when the wound is stuck in an inflammatory phase. To heal properly, wounds must be moved from the inflammatory phase to the proliferative phase. And if wounds persist and become chronic, resolution will be challenging. Other factors like multiple chronic comorbidities such as under-controlled diabetes mellitus, autoimmune disorders, untreated hypertension, untreated peripheral vascular disease, and poor nutrition can also create more challenges.
If not managed, chronic, infected wounds can progress to systemic infections that may require hospital admission and/or IV antibiotic infusions. Untreated systemic infections can lead to life-threatening septicemia, osteomyelitis (infection of the bone), the need for long-term antibiotics, or even surgery. Osteomyelitis has its own possible complications including septic arthritis and osteonecrosis (death of the bone). These complications put the patient at risk for amputation.
The signs and symptoms to report
Because purulent drainage is a sign of infection, it’s essential to recognize and report early signs so earlier diagnosis and treatment can occur. The goal is to effectively treat infected wounds before the infection advances to a more severe stage. Symptoms of infection that should be reported are:
- Fever
- Redness
- Warmth
- Edema
- Increased pain
- Chills
- Induration
- Nausea/vomiting
- Foul odor
- Worsening wound appearance or new tunnels to the wound
A thorough wound assessment and frequent monitoring for these signs and symptoms are crucial in preventing significant complications and wound deterioration, especially with purulent drainage present. If a patient on an oral antibiotic exhibits new signs of infection or signs of a deteriorating wound, an oral antibiotic review or intravenous antibiotics may be indicated.
For more persistent infections, the expertise of several specialty disciplines may be needed. For instance, general surgeons, orthopedic surgeons, vascular surgeons, infectious disease clinicians, and surgical podiatrists all have fundamental roles in treating difficult infections and their complications.
A referral to one of these specialists may be necessary. However, outpatient infusion care for patients that do not require hospital admission for IV antibiotics can also be an option. Likewise, outpatient wound care clinics are helpful in treating local infection and establishing an individualized wound treatment plan.
Remember that wounds with purulent drainage are never normal. This type of exudate should be evaluated as soon as possible to heal safely and successfully.
Elevate your expertise with our Skin and Wound Management course.
Get StartedWhat do you think?